Why Gut Health Matters in Babies
Your baby’s gut is home to trillions of microbes (bacteria, viruses, and fungi) collectively called the gut microbiome. In early life, this microbiome helps “train” the immune system, supports digestion, and contributes to the gut barrier that protects against irritation and infection. The first months are a particularly sensitive window because the microbiome is rapidly developing and responding to feeding, environment, illness, and medications.
Parents often hear that “C-section babies have different gut bacteria.” That’s partly true—especially early on—but it doesn’t mean your child is destined for poor health. Microbiomes change quickly, and many factors (especially feeding and antibiotic exposure) have a powerful influence over time.
C-Section vs. Vaginal Birth: What’s Different for the Microbiome?
How babies are colonized at birth
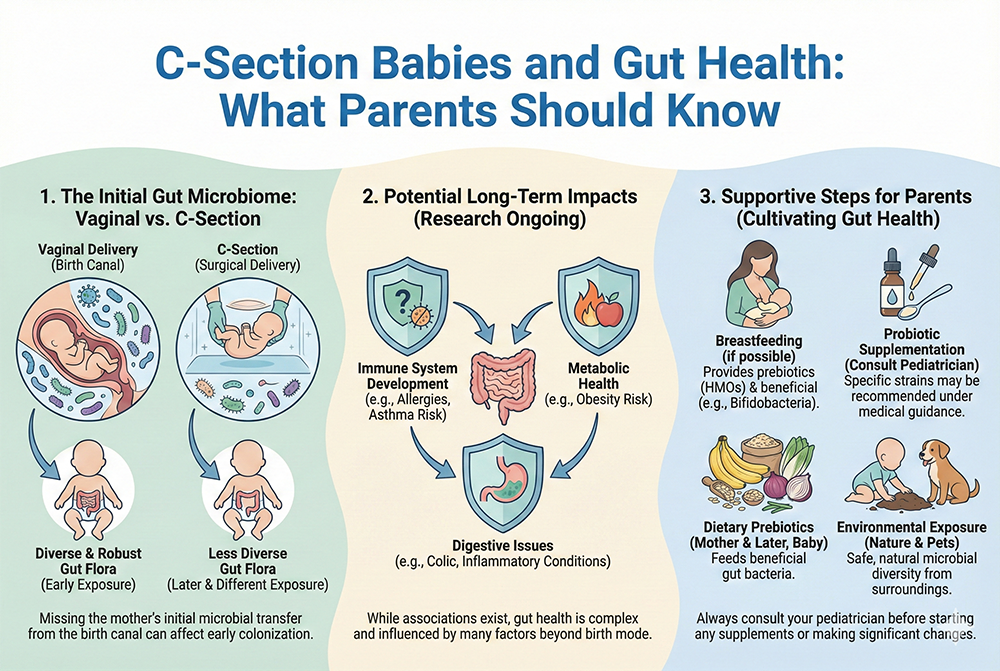
During a vaginal birth, a baby is exposed to microbes from the birthing parent’s vaginal and intestinal flora and from close skin-to-skin contact afterward. In a cesarean birth (C-section), early exposure is more influenced by skin microbes from caregivers and the hospital environment. This difference can lead to distinct patterns in the first days and weeks.
What studies generally show
Research consistently finds that, on average, babies born by C-section may have:
- Lower early levels of certain beneficial bacteria, including Bifidobacterium (often associated with breastfed infant guts) and Bacteroides (commonly seen after vaginal birth).
- Different early microbial diversity and timing of colonization, with a greater proportion of skin-associated microbes early on.
- A stronger impact from antibiotics, because C-sections often involve prophylactic antibiotics for the birthing parent, and sometimes antibiotics for the baby depending on the clinical situation.
It’s important to interpret these findings with care. Differences tend to be most noticeable in the early months and often become less pronounced over time, especially when babies receive human milk and have typical exposures at home.
Does This Difference Affect Health Outcomes?
Scientists are still untangling what early microbiome differences mean for long-term health. Many studies show associations between C-section birth and slightly higher risks of certain conditions, but association is not the same as causation. Other factors—genetics, the reason for the C-section, maternal health, antibiotics, feeding, and environment—can contribute.
Conditions that have been studied
Research has explored links between C-section birth and:
- Allergies and eczema
- Asthma
- Some gastrointestinal infections in early childhood
- Higher odds of overweight/obesity in some populations
The increased risks, when found, are typically modest at the individual level. Many C-section babies never develop these conditions, and many vaginally born children do. The microbiome is one piece of a much larger puzzle.
What matters most: the “whole context”
The reason the C-section happened (planned vs. emergency), maternal health (such as diabetes or obesity), exposure to antibiotics, prematurity, NICU stay, and feeding patterns can all influence gut microbes and immune development. A supportive plan after birth can make a meaningful difference regardless of delivery mode.
Key Factors That Shape a C-Section Baby’s Gut Microbiome
1) Antibiotics around birth
Antibiotics can be lifesaving and are often appropriate during a C-section to prevent infection. They can also temporarily reduce bacterial diversity and delay colonization of certain beneficial microbes. This effect varies widely among babies and typically shifts as feeding and everyday exposures continue.
2) Breast milk and human milk feeding
Human milk is one of the strongest microbiome supporters in infancy. It contains:
- Prebiotics (human milk oligosaccharides, or HMOs) that feed beneficial bacteria, especially Bifidobacterium.
- Antibodies and immune factors that help protect the gut lining.
- Beneficial bacteria that may contribute to the infant microbiome.
Exclusive breastfeeding is not the only path to a healthy microbiome. Partial breastfeeding and any amount of human milk can be helpful. If breastfeeding isn’t possible or desired, formula-fed babies can still develop a healthy microbiome, particularly with attentive feeding, responsive care, and appropriate medical guidance.
3) Skin-to-skin contact and close caregiving
Early and frequent skin-to-skin contact supports bonding, breastfeeding initiation, temperature stability, and may influence microbial exposure. For C-section births, where immediate contact may be delayed, asking about options for early skin-to-skin in the operating or recovery room can be valuable when medically appropriate.
4) Prematurity and NICU care
Preterm babies and babies needing NICU care often have different microbiome patterns due to medical interventions, sterile environments, and higher antibiotic exposure. If this is your situation, it doesn’t mean you’ve missed a window—it simply means gut support may look more individualized and medically guided.
5) Home environment and siblings
Everyday life matters. Living with siblings, being exposed to pets, spending time outdoors, and ordinary family contact can diversify microbial exposure. Balance is key: good hygiene practices without excessive sterilization support health and reduce unnecessary stress.
Practical, Evidence-Based Ways to Support Gut Health After a C-Section
If you’re a parent wondering what you can do now, focus on supportive steps that are safe, realistic, and backed by evidence.
Prioritize feeding support (whatever your feeding method)
- Seek early lactation support if breastfeeding is your goal. C-section recovery, pain control, and delayed milk “coming in” can make the start feel harder, but many families succeed with the right help.
- Offer human milk when possible. If direct nursing isn’t working, pumping, combination feeding, or donor milk (when available and appropriate) may be options.
- Use responsive feeding with bottle-feeding: paced feeds, watching hunger/fullness cues, and avoiding pressure can support digestion and comfort.
Ask about gentle, early skin-to-skin
When medical circumstances allow, skin-to-skin in the recovery room (or even in the operating room in some hospitals) can be a helpful start. If the birthing parent isn’t able immediately, a partner can often provide skin-to-skin.
Be thoughtful about antibiotics (but don’t fear them)
Never decline medically indicated antibiotics out of fear for the microbiome. Instead, you can ask informed questions, such as:
- “Is this antibiotic necessary right now?”
- “Is there a narrower option appropriate for this infection?”
- “What signs should I watch for after antibiotics (diarrhea, rash, thrush)?”
If your baby or you need antibiotics, gut microbes often rebound over time—especially with supportive feeding and normal life exposures.
Consider probiotics only with professional guidance
Parents often ask about infant probiotics for C-section babies. The evidence is promising for certain strains in specific situations (for example, some probiotics may reduce the risk of antibiotic-associated diarrhea, and particular strains have been studied for colic or eczema risk reduction). But probiotic effects are strain-specific, and products vary widely in quality.
Discuss probiotics with your pediatrician, particularly if your baby is premature, immunocompromised, has a central line, or is medically fragile—these babies require extra caution. If your clinician recommends a probiotic, ask which strain(s), dose, and duration are supported for your baby’s needs.
Skip DIY “vaginal seeding”
You may have heard of swabbing a C-section baby with vaginal fluids to mimic vaginal birth exposure. Major medical organizations generally advise against DIY vaginal seeding outside of research settings due to infection risks (including group B strep, herpes, chlamydia, and other pathogens that may be present without symptoms). If you’re interested, ask your care team about the current evidence and safety considerations.
Support a calm, gut-friendly routine
- Protect sleep as best you can—sleep disruption can affect digestion and immune function for both baby and parents.
- Use soothing strategies for reflux-like symptoms or gassiness: upright holding after feeds, paced bottle-feeding, gentle burping, and discussing persistent symptoms with your pediatrician.
- Choose smoke-free environments. Tobacco smoke exposure is linked with higher risks of respiratory illness and can affect overall health and immune development.
What to Expect: Poop, Gas, and Common Gut Concerns
Is C-section gas or colic real?
Many parents feel their C-section baby is gassier or fussier. Some studies suggest differences in early gut colonization might influence gassiness or crying patterns, but colic is multifactorial and very common across birth modes. If your baby is thriving, gaining weight, and has no red flags, mild gas and fussiness are often part of normal infant development.
Normal stool patterns vary widely
Stool frequency and color change based on age and feeding method. Breastfed babies can poop many times a day or go several days between stools once breastfeeding is established. Formula-fed babies often have more regular, pastier stools. What matters most is your baby’s overall comfort, growth, hydration, and whether stools contain blood or are persistently pale/white.
When to call the pediatrician
Seek medical advice promptly if your baby has:
- Fever (especially in babies under 3 months, which needs urgent guidance)
- Blood in stool
- Persistent vomiting (especially green/bilious vomit)
- Signs of dehydration (fewer wet diapers, very sleepy, dry mouth)
- Severe eczema, wheezing, or poor weight gain
Starting Solids: Building a Healthy Gut After 6 Months
The transition to solid foods is a major microbiome milestone—often bigger than the mode of delivery in the long run. Around 6 months (and when your baby shows readiness signs), you can support gut health by offering a variety of whole foods over time.
Focus on fiber-rich, diverse foods
Fiber feeds beneficial gut bacteria. Age-appropriate options include:
- Vegetables and fruits (soft-cooked sticks, mashed, purées, or small safe pieces)
- Legumes (well-cooked lentils, beans mashed smooth)
- Whole grains (oatmeal, whole wheat pasta cooked soft)
Include allergen foods early and safely
Introducing common allergens (like peanut, egg, dairy, wheat) in age-appropriate forms during the first year may reduce allergy risk for many babies, especially when introduced after a few low-risk foods are tolerated. If your baby has severe eczema or known food allergy, ask your pediatrician or allergist for a personalized plan.
Limit ultra-processed foods and added sugars
Highly processed foods can crowd out the variety of plant fibers that support microbial diversity. You don’t need perfection—just aim for a pattern that favors minimally processed foods most of the time.
Supporting the Birthing Parent Supports the Baby, Too
C-section recovery is real recovery. Pain control, rest, nutrition, hydration, and emotional support help the birthing parent heal and can make feeding and bonding easier.
Gentle recovery tips that can indirectly support gut health
- Take pain management seriously. Adequate pain control can improve mobility, sleep, and breastfeeding comfort. Discuss options that fit your situation.
- Eat nourishing meals with protein, fiber, and fluids to support healing and bowel regularity after surgery.
- Accept help so you can rest, feed the baby, and recover.
If you’re feeling persistent sadness, anxiety, intrusive thoughts, or overwhelm, reach out to your healthcare provider. Parental mental health is a vital part of family wellness.
The Bottom Line: Is There a Difference—and What Should Parents Do?
Yes, C-section babies often have a somewhat different early gut microbiome compared with vaginally born babies—especially in the first weeks to months. But this is not a verdict on your child’s future health. Microbiomes are dynamic, and the factors you can influence—feeding support, skin-to-skin contact, thoughtful antibiotic use, a varied diet when solids begin, and a healthy home environment—can meaningfully support gut development.
If you’re reading this because you had (or will have) a C-section, you haven’t “missed your chance.” You’ve brought your baby into the world, and there are many warm, practical steps you can take from here.