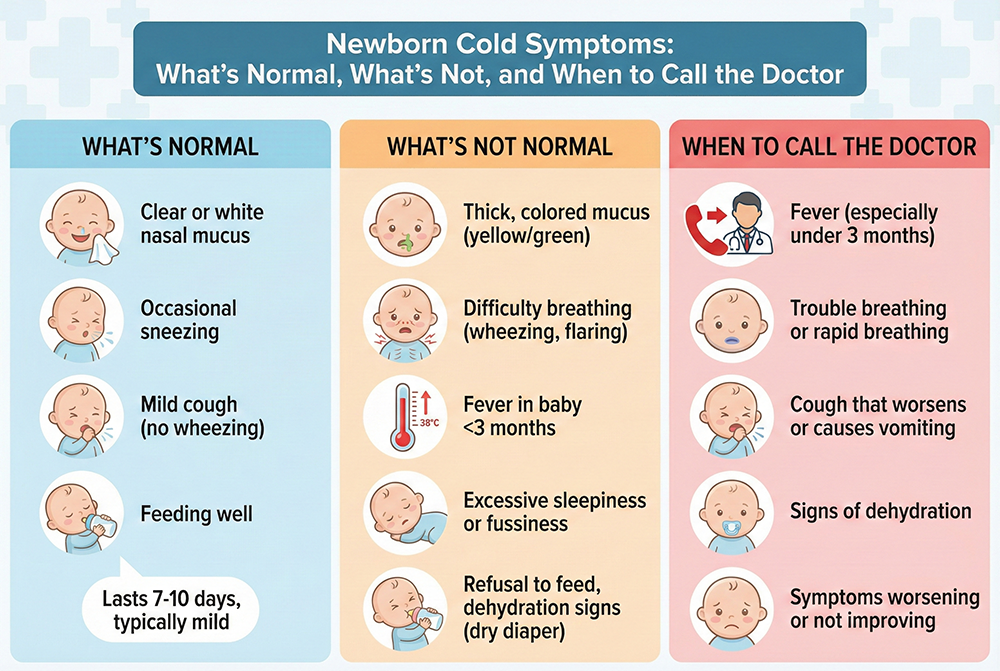
Understanding Newborn Cold Symptoms
Hearing your newborn sniffle or watching them struggle with a stuffy nose can be stressful—especially in the first weeks of life. Most “colds” in newborns are caused by common respiratory viruses and are usually mild, but newborns (under 28 days old) have immature immune systems and smaller airways. That means symptoms can feel more dramatic, and certain signs require faster medical attention.
A “cold” is an upper respiratory infection (URI) that typically affects the nose and throat. In newborns, even a small amount of mucus can interfere with feeding and sleep because babies are primarily nose-breathers. While many babies recover with supportive care, it’s important to know what’s typical, what might be something else (like allergies or reflux), and when to call your pediatrician.
Common Cold Symptoms in Newborns
Newborn cold symptoms often look similar to older children’s symptoms, but they may be subtler—or show up as feeding and behavior changes rather than obvious complaints.
Nasal congestion and runny nose
Congestion is one of the most common newborn cold symptoms. You may notice:
- Sniffling or “snorting” sounds
- Clear to cloudy mucus
- Noisy breathing, especially when lying flat
Clear mucus can occur early in a viral illness; thicker, cloudy mucus can appear as symptoms progress. Mucus color alone does not reliably tell you if an infection is viral or bacterial.
Sneezing
Sneezing is common and not always a sign of illness. Newborns sneeze to clear mucus, milk, and normal environmental particles from their tiny nasal passages. Frequent sneezing with congestion or cough is more suggestive of a cold.
Cough
A mild cough can happen as mucus drips down the throat (postnasal drip). Newborn coughs should be taken seriously if they are persistent, worsening, or accompanied by breathing difficulty. A cough in a very young baby is a reason to check in with your pediatrician, especially if your baby is under 2 months.
Low-grade fever or temperature changes
Some babies develop a mild temperature elevation with a viral infection. However, in newborns, any fever can be significant. A rectal temperature of 100.4°F (38°C) or higher in a baby under 3 months requires prompt medical evaluation—regardless of how “well” they look.
Feeding changes
Congestion can make it hard for a newborn to coordinate breathing and feeding. Signs include:
- Shorter feeds
- Frequent unlatching or pulling off the bottle/breast
- Increased spit-up
- Fussiness during feeds
Hydration is a key marker of how well a baby is coping with illness.
Sleep disruption and irritability
Newborns often sleep more when they’re sick, but they may also wake more due to congestion. Increased fussiness can happen because they’re uncomfortable and tired.
What Causes Cold-Like Symptoms in Newborns?
Not every sniffle is a cold. Understanding the common causes can help you respond appropriately.
Viral upper respiratory infections (most common)
Viruses such as rhinovirus, seasonal coronaviruses (not only COVID-19), RSV, parainfluenza, and others can cause typical cold symptoms. Newborns often catch viruses from siblings, caregivers, or visitors who have mild symptoms.
Dry air and normal newborn congestion
Many newborns sound congested even when they’re not sick. Dry indoor air, dust, and small nasal passages can cause “normal” congestion. If there’s no fever, no cough, and your baby feeds well, simple measures like humidification and saline drops may be all that’s needed.
Reflux (GER/GERD)
Spit-up and reflux can cause throat irritation, coughing, and noisy breathing. Reflux symptoms often worsen after feeds and when lying flat.
Allergies (less common in newborns)
True seasonal allergies are uncommon in very young infants. However, irritants such as smoke, strong fragrances, and pet dander can contribute to nasal symptoms.
More serious infections
In newborns, what seems like a cold can occasionally be an early sign of a more serious infection. This is why fever and breathing changes require careful attention.
When Newborn Cold Symptoms Are an Emergency
Trust your instincts. If something feels “off,” it’s always appropriate to seek care. Use the guidance below to decide how urgently to act.
Call your pediatrician urgently or seek emergency care if your newborn has:
- Fever: rectal temp 100.4°F (38°C) or higher in a baby under 3 months
- Breathing difficulty: fast breathing, struggling for air, grunting, flaring nostrils, or chest retractions (skin pulling in between ribs or at the collarbone)
- Color changes: lips/face turning blue or gray, or very pale/mottled skin
- Poor feeding: refusing feeds or significantly reduced intake
- Dehydration signs: fewer wet diapers (often fewer than 6 per day after the first week), dry mouth, no tears when crying (older infants), or sunken soft spot
- Unusual sleepiness: difficult to wake, very floppy, or less responsive
- Persistent vomiting or vomit that is green (bilious)
- Apnea: pauses in breathing
- Symptoms in a high-risk baby: premature infants, babies with heart/lung conditions, or immune concerns
Breathing rate quick check
Newborn breathing can be irregular, but sustained rapid breathing is concerning. If your baby is consistently breathing very fast (often over about 60 breaths per minute at rest), working hard to breathe, or you see retractions, seek medical care.
When to Call the Doctor (Non-Emergency but Important)
Contact your pediatrician for advice if your newborn has:
- Cold symptoms lasting more than 7–10 days or worsening after initial improvement
- A cough that becomes frequent, harsh, or disrupts feeding
- Wheezing or a whistling sound when breathing
- Eye discharge with redness or swelling
- Ear tugging with increased fussiness (ear infections are less common in newborns but possible)
- Any fever concerns even below 100.4°F if your baby is under 2 months and seems unwell
Safe, Evidence-Based Home Care for Newborn Cold Symptoms
For most uncomplicated colds, treatment is supportive. The goal is to help your baby breathe, feed, and rest comfortably while the virus runs its course.
1) Clear the nose (the most helpful step)
Because newborns rely heavily on nasal breathing, clearing congestion can dramatically improve feeding and sleep.
- Saline drops or saline mist: Place 1–2 drops in each nostril to loosen mucus.
- Gentle suction: Use a bulb syringe or nasal aspirator after saline. Suction just enough to help your baby feed—over-suctioning can irritate the nasal lining.
- Best times: Before feeds and before sleep.
2) Use humidified air
A cool-mist humidifier can help loosen mucus and reduce throat irritation. Clean it daily as directed to prevent mold and bacterial growth. If you don’t have a humidifier, sitting with your baby in a steamy bathroom for a few minutes (not hot steam directly on baby) can sometimes help with congestion.
3) Keep feeds frequent and watch hydration
Offer breast milk or formula more often if your baby is taking smaller volumes due to congestion. Hydration supports recovery and helps thin secretions.
Practical markers:
- Wet diapers (frequency and heaviness)
- Alertness during wake windows
- Moist lips and mouth
4) Support better sleep safely
It’s tempting to use inclined sleepers or prop the mattress, but the safest sleep recommendations remain the same even when your baby has a cold:
- Back to sleep for every sleep
- Firm, flat sleep surface
- No pillows, wedges, loose blankets, or sleep positioners
To help comfort without changing sleep safety, try clearing the nose before sleep, using a humidifier, and offering extra cuddles during awake time.
5) Keep your newborn comfortable
- Dress in light layers and keep the room at a comfortable temperature.
- Gentle soothing: rocking, skin-to-skin, and quiet contact can reduce stress and help regulate breathing.
- Minimize irritants: avoid smoke exposure (including thirdhand smoke on clothing), strong fragrances, and aerosol sprays.
Medications and Remedies to Avoid in Newborns
Many over-the-counter products marketed for colds are not safe for newborns. When in doubt, ask your pediatrician before giving anything by mouth or applying medicated rubs.
Avoid these unless specifically directed by a clinician:
- OTC cough and cold medicines: Not recommended for infants; they can cause serious side effects and do not reliably help.
- Honey: No honey (including in teas or remedies) for babies under 12 months due to botulism risk.
- Essential oils: Many are unsafe for infants and can irritate the airways; ingestion is dangerous.
- Mentholated rubs: Can irritate and may worsen breathing in young infants.
- Leftover antibiotics: Antibiotics do not treat viral colds and inappropriate use can be harmful.
What about fever reducers?
If your newborn is under 3 months and has a fever (100.4°F/38°C or higher), do not treat at home first—seek medical evaluation promptly. For babies older than that, clinicians often recommend acetaminophen based on weight, but dosing in young infants should be guided by a pediatrician.
How Long Do Newborn Colds Last?
A typical viral cold lasts about 7–10 days. Congestion often peaks around days 2–4, then gradually improves. A mild cough can linger longer as the airway heals.
Call your pediatrician if symptoms persist beyond 10 days, if your baby worsens after improving, or if feeding and breathing become more difficult.
How to Tell a Cold from RSV, Flu, or COVID-19
Many respiratory viruses look alike in the beginning. Testing is sometimes needed to know the exact cause, especially in young infants. The most important factor is not the name of the virus but how your baby is breathing, feeding, and behaving.
RSV (Respiratory Syncytial Virus)
RSV can start like a cold and then move into the lower airways. Watch for:
- Worsening cough
- Wheezing or noisy breathing
- Rapid breathing or retractions
- Feeding difficulty due to shortness of breath
Influenza (flu)
Flu may cause more sudden, significant illness with higher fever (though fever isn’t always present). Babies can appear more tired and uncomfortable.
COVID-19
COVID-19 in infants can range from mild to more symptomatic. Signs can include congestion, fever, cough, and feeding changes. Follow your pediatrician’s guidance on testing and isolation, especially to protect vulnerable family members.
Preventing Colds in Newborns (Realistic, Effective Steps)
You can’t prevent every germ, but you can reduce risk—especially during the newborn period.
Hand hygiene and visitor boundaries
- Wash hands with soap and water before holding the baby.
- Use alcohol-based sanitizer when soap isn’t available.
- Ask visitors to skip the visit if sick, even with “just allergies.”
- Avoid kissing the baby’s face and hands, which easily transfer viruses.
Limit exposure in peak seasons
During high respiratory virus seasons, consider avoiding crowded indoor spaces with your newborn when possible, especially in the first 4–8 weeks.
Keep the air clean
- No smoking or vaping around the baby.
- Reduce strong scents and aerosols.
- Maintain a comfortable humidity level (often around 40–50%).
Breastfeeding support (if applicable)
Breast milk provides antibodies and immune support that can reduce the risk or severity of some infections. If breastfeeding is part of your feeding plan and your baby is sick, frequent feeds can offer both hydration and comfort.
Vaccines and protective strategies around baby
Newborns are too young for many vaccines, so protection often comes from the people around them. Keeping parents, siblings, and caregivers up to date on recommended vaccines (such as flu and whooping cough/Tdap, as advised by your clinician) can help create a safer “cocoon” around your baby.
Newborn Cold Symptoms at Night: A Practical Plan
Nights can feel longer when your baby is congested. A simple routine can help:
- Before bedtime feed: saline + gentle suction, then feed.
- During the night: if baby wakes struggling to feed, pause and clear the nose again.
- Humidifier on: keep it running with clean, fresh water.
- Monitor breathing: if you see retractions, rapid breathing, grunting, or color changes, seek urgent care.
When You’re Worried: What to Track for the Pediatrician
If you call your pediatrician, having a few details ready can make the conversation clearer:
- Baby’s age and any prematurity or medical conditions
- Temperature and how you took it (rectal is most accurate in infants)
- Feeding amount and frequency in the past 24 hours
- Number of wet diapers
- Breathing observations (fast breathing, retractions, wheeze, pauses)
- How long symptoms have been present and whether they’re improving or worsening
- Known exposures (sick siblings/contacts)
Reassurance for Parents
Most newborn colds are manageable with supportive care, and it’s normal to feel anxious when your baby sounds congested. Focus on the big three: breathing, feeding, and hydration. If your baby is breathing comfortably, taking feeds reasonably well, and making wet diapers, you’re likely on the right track.
And if you’re unsure—especially in the first month—calling your pediatrician is never an overreaction. Newborns change quickly, and you deserve clear guidance and peace of mind.