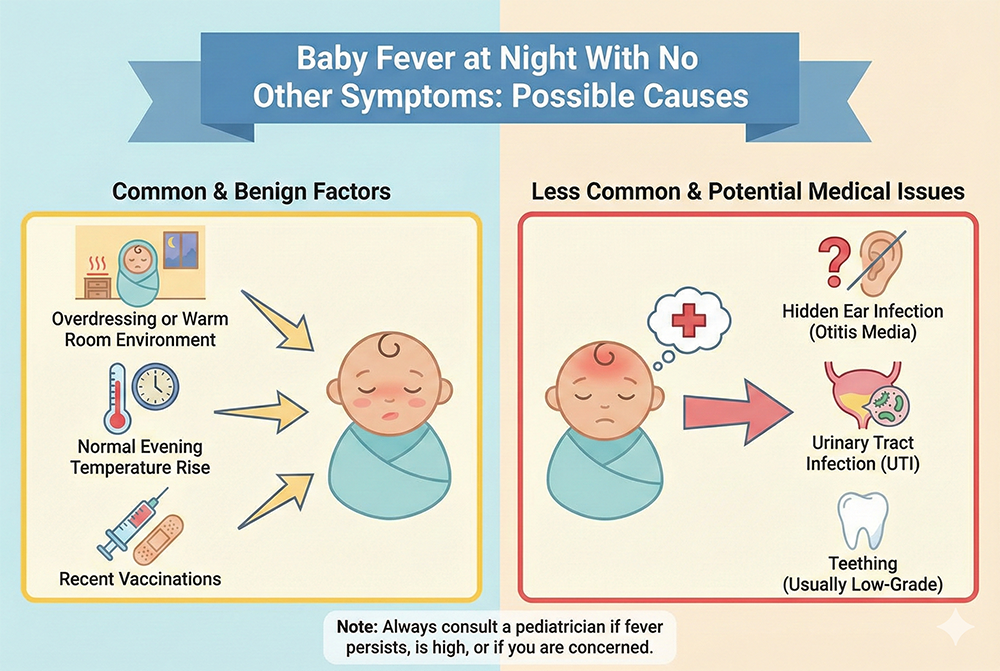
Why a Baby May Have a Fever Only at Night
It can be unsettling to check on your baby at bedtime and find they feel warm—especially when they seem perfectly fine during the day. A baby fever with no other symptoms at night is fairly common, and in many cases it’s not an emergency. There are several reasons temperatures can rise in the evening, and not all of them are due to serious illness.
Body temperature naturally follows a daily rhythm (called a circadian rhythm). Many people—babies included—tend to run slightly warmer in the late afternoon and evening than in the early morning. On top of that, babies have developing temperature regulation, which means they can heat up faster than older children, especially if they’re overdressed or the room is warm.
Still, fever is also a sign that the immune system is responding to something. The key for parents is to measure the temperature accurately, assess how your baby looks and behaves, and know when to seek medical advice.
What Counts as a Fever in Babies?
Before you decide what to do, it helps to define fever correctly. A baby can feel warm without having a true fever. The most reliable way to know is to use a thermometer.
Fever thresholds (general pediatric guidance)
- Rectal temperature: Fever is typically 100.4°F (38.0°C) or higher. This is considered the most accurate method for infants.
- Forehead (temporal) scan: Can be useful, but results may vary based on technique and environment. Confirm a high reading with a more accurate method if possible.
- Armpit (axillary) temperature: Often reads lower; may be used for screening, but confirm if elevated.
- Ear (tympanic) temperature: Accuracy depends on age and proper placement; less reliable in very young babies.
Important: In babies under 3 months, a temperature of 100.4°F (38.0°C) or higher is more urgent and should prompt a call to a healthcare professional right away, even if there are no other symptoms.
Common Reasons for Nighttime Fever With No Other Symptoms
If your baby has a fever at night and seems otherwise normal—eating reasonably well, breathing comfortably, and able to be soothed—these are some of the most common explanations.
1) Normal daily temperature variation
It’s normal for body temperature to peak later in the day. A baby whose temperature is borderline in the evening may be back to normal by morning. If the temperature is only mildly elevated and your baby is comfortable, this can be part of normal physiology.
2) Overheating from sleep environment
Babies can overheat easily due to:
- Too many clothing layers or heavy sleep sacks
- Thick blankets (not recommended for infants)
- A room that’s too warm
- Close contact in bed-sharing situations (and bed-sharing also increases other risks)
Overheating can make a baby feel hot and sweaty and may raise measured temperature. If your baby is warm but otherwise well, check the room temperature and clothing. A comfortable room for sleep is often around 68–72°F (20–22°C), though comfort can vary by home and season.
3) Early viral illness (before other symptoms appear)
Many viral infections begin with fever as the first noticeable sign. Congestion, cough, diarrhea, or rash may not appear until 12–48 hours later. In this case, the fever may be more noticeable at night when your baby is at rest and you’re checking them more closely.
4) Recent vaccinations
After routine immunizations, some babies develop a low-grade fever within 24–48 hours (timing can vary by vaccine). Often, fever may show up at night and your baby may otherwise look well. If your baby recently had shots, check the vaccine handout or ask your pediatrician what to expect and how to manage discomfort.
5) Teething (what it can and can’t do)
Teething can cause drooling, gum discomfort, irritability, and changes in sleep. It may cause a slight temperature rise, but evidence suggests teething does not typically cause a true fever (100.4°F/38°C or higher). If your baby has a real fever, it’s wise to look beyond teething as the main cause.
6) Mild dehydration
If your baby hasn’t been taking in as many fluids—due to busy days, feeding changes, or mild illness—dehydration can contribute to feeling warm and can worsen discomfort. Dehydration doesn’t usually cause a high fever by itself, but it can make a baby seem more unwell. Watch for fewer wet diapers, dry mouth, and lethargy.
7) Less obvious infections (sometimes with few symptoms)
Some infections can cause fever with minimal early symptoms, especially in infants. Examples include:
- Urinary tract infection (UTI): May cause fever without cough or congestion. Sometimes there’s fussiness, feeding changes, or foul-smelling urine, but not always.
- Ear infection: Some babies don’t tug ears. Night waking, fussiness lying down, and fever can be clues.
- Roseola: Often causes several days of fever with few other symptoms, followed by a rash as the fever breaks (typically in older infants/toddlers).
If your baby repeatedly has fever with no obvious source, especially under 12 months, a clinician may consider urine testing or further evaluation.
How to Check Your Baby’s Temperature Accurately at Night
Nighttime checks are often rushed or done in dim light, which can lead to inconsistent readings. Accuracy matters because fever thresholds guide what to do next.
Best practices
- Use the right tool: For infants, a digital rectal thermometer is often considered the most accurate. Follow your pediatrician’s guidance and the device instructions.
- Confirm unusual readings: If a forehead scan shows a fever but your baby seems fine, consider rechecking with a more reliable method.
- Wait after a bath or feeding: Recent warm baths, vigorous crying, or bundled feeding can temporarily raise skin temperature.
- Record the details: Note the time, method (rectal/forehead/armpit), and the number. This helps your pediatrician interpret trends.
What to Do at Home Tonight (Step-by-Step)
If your baby has a fever at night but no other symptoms, focus on comfort, hydration, and monitoring.
1) Look at your baby, not just the number
Ask yourself:
- Are they difficult to wake or unusually limp?
- Are they breathing comfortably?
- Can they be consoled?
- Are they drinking and making wet diapers?
A baby who is alert at times, feeding reasonably, and has normal breathing is often safe to monitor closely at home—unless they’re very young (see “When to call” below).
2) Adjust the sleep environment
- Dress your baby in one light layer more than an adult would wear for comfort.
- Avoid hats indoors during sleep.
- Use a sleep sack instead of blankets for infants.
- Keep the room comfortably cool and well ventilated.
3) Offer fluids and continue feeding
For babies, hydration usually means breast milk or formula. Offer feeds a bit more frequently if your baby is willing. For older babies already taking solids, you can still prioritize milk feeds; small sips of water may be appropriate depending on age and your pediatrician’s advice.
4) Consider fever medicine only if needed for comfort
Fever itself is not always dangerous; it’s often part of the body’s immune response. The goal of medication is comfort—helping your baby rest, drink, and settle.
- Acetaminophen (paracetamol): Commonly used for infants, with dosing based on weight.
- Ibuprofen: Generally used for babies 6 months and older, with weight-based dosing.
Safety notes: Always follow your pediatrician’s guidance and the label instructions. Use the dosing syringe/cup that comes with the medication. Avoid using multiple combination products. Do not give aspirin to children due to the risk of Reye’s syndrome.
5) Avoid alcohol rubs and cold baths
Cold water baths can cause shivering, which may raise the internal temperature and increase discomfort. Alcohol rubs are unsafe because alcohol can be absorbed through skin and inhaled.
6) Monitor and recheck strategically
You don’t need to wake a comfortably sleeping baby just to recheck a mild fever—unless advised by your clinician or your baby is under 3 months. If your baby is sleeping peacefully, you can check breathing and comfort and recheck temperature when they naturally wake.
When to Call the Doctor or Seek Urgent Care
Use age and overall appearance to guide urgency. If you’re ever unsure, it’s appropriate to contact a pediatrician or nurse line—especially for young infants.
Call urgently (same night) or seek emergency care if:
- Your baby is under 3 months and has a temperature of 100.4°F (38.0°C) or higher.
- Your baby has trouble breathing, fast breathing, grunting, persistent wheezing, or bluish lips/face.
- Your baby is hard to wake, very floppy, unusually weak, or not making eye contact when awake.
- There are signs of dehydration: very few wet diapers, no tears when crying, dry mouth, or sunken soft spot (fontanelle).
- Your baby has a seizure, including a febrile seizure (call emergency services).
- Your baby has a stiff neck, severe headache (older baby/toddler cues may include extreme irritability), or sensitivity to light.
- You see a purple/petechial rash (small purple/red spots that don’t blanch when pressed) or any rapidly spreading rash with fever.
- Your baby has a high fever (for example, 104°F/40°C or higher) or looks very ill regardless of the number.
- Fever follows being left in a hot environment or you suspect heat illness.
Call your pediatrician within 24 hours if:
- Your baby is 3–6 months with fever, even if otherwise well (many clinics want to advise on next steps).
- Fever lasts more than 24 hours in a baby under 2 years without an obvious source.
- Fever lasts more than 3 days in any child.
- Your baby has recurrent nighttime fevers with no clear symptoms.
- Your baby has pain, persistent fussiness, feeding refusal, or you suspect an ear infection or UTI.
- Your baby has a chronic medical condition or is immunocompromised.
Could It Be a UTI If There Are No Other Symptoms?
Yes—especially in infants. A urinary tract infection can present as fever with no cough, no runny nose, and no obvious source. UTIs are more likely if your baby is under 12 months, uncircumcised male (in early infancy), has a history of UTIs, or has urinary tract abnormalities (if known).
Signs can be subtle:
- Fever
- Fussiness or poor sleep
- Poor feeding
- Vomiting
- Foul-smelling urine (not always present)
If a UTI is suspected, your clinician may recommend a urine sample. Early diagnosis matters because untreated UTIs can lead to kidney infection.
How to Support Rest When Your Baby Has a Nighttime Fever
Sleep often gets disrupted with fever, even when there are no other symptoms. These strategies can help your baby rest and help you feel more in control.
Comfort measures that often help
- Keep routines gentle: Dim lights, soft voice, slow movements.
- Use soothing contact: Rocking, holding, or patting can reduce stress hormones and help baby settle.
- Clear nasal passages if needed: If mild congestion begins, saline drops and gentle suction can help before feeds and sleep.
- Offer smaller, more frequent feeds: This supports hydration without overwhelming a tired baby.
What not to do
- Don’t force your baby to eat solids during fever; focus on fluids.
- Don’t overdress to “sweat it out.” Overheating can worsen discomfort.
- Don’t rely on touch alone; always confirm fever with a thermometer.
Tracking Patterns: A Simple Fever Log Parents Can Use
If your baby’s fever seems to happen mostly at night, a short log can be extremely useful for your pediatrician. Include:
- Date and time of temperature
- Temperature reading and method used
- Baby’s behavior (playing, fussy, sleepy but rousable)
- Feeding amounts and wet diapers
- Any medication given (name, dose, time)
- New exposures (daycare illness, travel, vaccination)
Patterns like “fever spikes at night, normal in morning” can occur with viral illness, but persistent or recurring patterns may warrant evaluation.
Prevention: Reducing the Chances of Nighttime Fever
You can’t prevent every fever—many are part of normal childhood immune development—but you can reduce risks and avoid overheating.
Practical prevention tips
- Hand hygiene: Wash hands after diaper changes and before feeds.
- Limit exposure to sick contacts: Especially for newborns and young infants.
- Follow the recommended vaccine schedule: Vaccination helps prevent serious infections that can cause high fever.
- Optimize sleep environment: Keep room temperature comfortable; avoid heavy bedding.
- Stay on top of hydration: Especially during hot weather or when baby is mildly ill.
Reassurance for Parents: Most Fevers Are Manageable
Hearing “fever” and “baby” in the same sentence can spike any parent’s anxiety—particularly at night when resources feel limited and everything seems more intense. The encouraging truth is that most fevers in babies and toddlers are caused by common viral infections and resolve with supportive care.
Your job isn’t to eliminate every fever; it’s to watch for red flags, keep your baby comfortable and hydrated, and reach out for help when the situation falls outside typical, safe boundaries. Trust your instincts. If your baby’s behavior worries you—even if the thermometer number isn’t dramatic—calling your pediatrician is a reasonable and responsible next step.