What “Sleep Through the Night” Really Means (and Why It’s Confusing)
Many parents picture “sleeping through the night” as a solid 10–12 hours with no waking. In baby sleep research and pediatric practice, it often means something much more modest: a 5–6 hour uninterrupted stretch. Some studies use 6–8 hours as the definition.
This matters because a breastfed baby who wakes once or twice to feed may be doing exactly what their biology is designed to do—especially in the first months. Babies have small stomachs, rapid brain growth, and lighter sleep cycles than adults. So when you ask, “When do breastfed babies sleep through the night?” the most accurate answer is: it varies widely, and night waking can be normal even when everything is going well.
Why breastfed babies may wake more often
- Breast milk digests quickly, so some babies feel hungry sooner compared with formula-fed peers.
- Frequent feeding protects milk supply in the early months, because milk production is regulated by demand.
- Normal developmental arousals happen as babies transition between sleep cycles; some babies resettle, others need help.
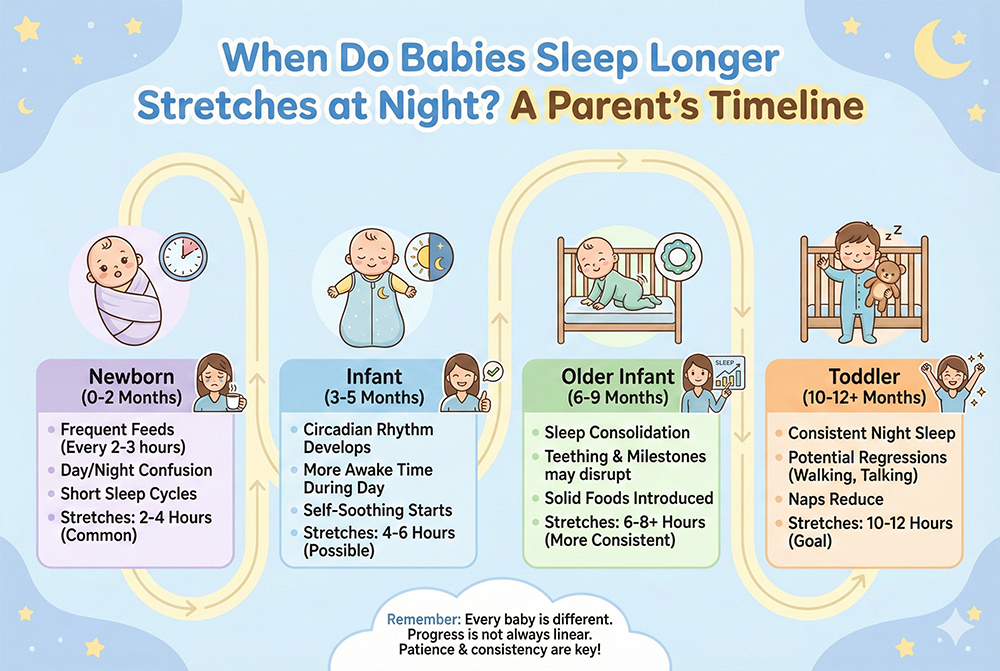
Typical Sleep Milestones for Breastfed Babies
There is no single “right” age when breastfed infants sleep through the night, but there are common patterns. Below are evidence-informed ranges you may hear from pediatric clinicians and lactation professionals. Remember: these are averages, not promises.
0–8 weeks: frequent waking is expected
In the newborn stage, many babies wake every 2–3 hours (sometimes more often) to feed. This is normal and protective. Newborns are also still sorting out day/night rhythms, and their sleep is fragmented.
What to aim for: adequate feeding, weight gain, safe sleep, and a sustainable plan for parental rest.
2–4 months: longer stretches may begin
Many breastfed babies start giving their longest stretch earlier in the night. Some may sleep a 4–6 hour stretch and then feed. Others continue frequent waking—especially during growth spurts or if reflux, eczema itching, or congestion is interfering with comfort.
What to aim for: consistent bedtime routine, plenty of daytime calories, and gradual differentiation between day and night.
4–6 months: some babies sleep 6–8 hours (but many don’t)
By this age, some infants—breastfed or not—are capable of longer stretches. But it’s also common for babies to keep at least one night feed. Developmental changes, teething discomfort, and increased awareness can all trigger more waking.
What to aim for: one or two predictable night feeds may be normal; consider gentle sleep-shaping strategies if frequent waking is exhausting your family.
6–12 months: “through the night” may happen—or night feeds may persist
Some breastfed babies naturally drop night feeds during this window. Others continue waking for feeding and connection. This can still be developmentally normal, especially if breastfeeding is also serving as comfort during separation anxiety, illness, travel, or major milestones like crawling and standing.
What to aim for: decide what “good sleep” means for your family, and choose strategies that align with your values and your baby’s temperament.
Factors That Affect When a Breastfed Baby Sleeps Through the Night
Two babies of the same age can have completely different sleep patterns and still be healthy. These factors often explain why.
1) Baby temperament and sleep biology
Some babies are naturally more sensitive to stimulation or have more difficulty transitioning between sleep cycles. This is not caused by breastfeeding; it’s part of individual variation.
2) Feeding effectiveness and daytime intake
If baby is not transferring milk well (for example due to latch issues, oral restrictions, or low supply), they may wake more often to meet calorie needs. On the other hand, many babies wake at night even with excellent intake—so frequent waking doesn’t automatically mean something is wrong.
Signs feeding is going well: steady growth, adequate wet diapers, contentment after most feeds, and your clinician’s reassurance.
3) Growth spurts and developmental leaps
Cluster feeding and increased waking often happen around common growth spurt periods (frequently cited around 3 weeks, 6 weeks, 3 months, and 6 months, though timing varies). Babies may temporarily need more calories or comfort.
4) Sleep associations
If baby usually falls asleep while nursing, they may look for the same conditions when they naturally wake between sleep cycles. This is not “bad”—it’s simply a pattern. You can keep it, or gently broaden baby’s settling skills if night waking is frequent and unsustainable.
5) Medical discomfort
Reflux, food allergies/intolerances, eczema itching, ear infections, and nasal congestion can all fragment sleep. If your baby’s waking seems painful or sudden, or there are feeding issues, talk with your pediatric clinician.
Night Waking: What’s Normal vs. When to Seek Help
It’s easy to worry that frequent waking means your baby “should” be sleeping through the night. In reality, night waking can be normal well into the first year (and beyond), especially for breastfed babies. What matters is whether your baby is thriving and your family is coping.
Normal patterns often include:
- 1–3 night wakings in the first 6 months
- Increased waking during illness, teething, travel, or big milestones
- Early-morning waking (around 4–6 a.m.) that feels like “the day is starting”
Consider checking in with a professional if you notice:
- Poor weight gain or fewer wet diapers than expected
- Feeding is painful, baby clicks or slips off frequently, or you suspect low milk transfer
- Loud snoring, pauses in breathing, or persistent mouth breathing
- Frequent vomiting, blood in stool, or signs of significant reflux discomfort
- Inconsolable crying or waking that seems driven by pain
- Parental mental health strain—if you feel depressed, anxious, or unsafe due to sleep deprivation, you deserve support quickly
How to Help a Breastfed Baby Sleep Longer (Gentle, Evidence-Based Strategies)
You don’t need extreme measures to improve sleep. Small, consistent changes often make the biggest difference—especially when paired with realistic expectations.
Prioritize safe sleep first
Always follow safe sleep guidance from your pediatric health authority. In general, the safest sleep setup is baby on their back, on a firm flat surface, with no loose bedding. If you are considering room-sharing or bed-sharing, get individualized, evidence-based guidance and assess risks carefully—especially if there is smoking, alcohol use, sedating medications, or an unsafe sleep surface.
1) Feed well during the day (without over-scheduling feeds)
Many breastfed babies do best with frequent daytime feeding. If your baby is easily distracted, try calmer feeds in a dim room. For some families, offering feeds every 2–3 hours during the day (and at least once before your bedtime) supports longer night stretches.
- Watch the baby, not the clock: hunger cues include rooting, hand-to-mouth, and fussing that escalates.
- Consider a “top-up” feed before you go to sleep, if it works for your baby.
2) Build a simple, consistent bedtime routine
Routines cue the brain that sleep is coming. Keep it short and repeatable:
- diaper change
- pajamas and sleep sack
- feed
- song or brief book
- white noise, dark room
- into sleep space
Consistency matters more than the exact steps.
3) Support circadian rhythm with light and timing
Babies learn day versus night through light exposure and routines. Helpful habits include:
- Morning daylight soon after waking
- Dim lights during evening feeds and night changes
- Keep night interactions boring: quiet voice, minimal eye contact, no play
4) Aim for age-appropriate wake windows (without obsessing)
Overtired babies may wake more often, but so can under-tired babies. If bedtime is a battle or night waking increases, gently adjust daytime naps or bedtime by 15–30 minutes for a few days and observe.
Tip: If your baby’s naps are very short, focus on soothing and consistency rather than trying to “force” longer naps right away.
5) Reduce unnecessary full awakenings at night
If your baby stirs, pause briefly before intervening. Many babies make noise between cycles and may resettle. If baby escalates, respond. This small pause can sometimes reduce full wake-ups without any crying-based training.
6) Consider “layering” sleep associations
If nursing to sleep is working for you, you can keep it. If you want baby to rely a little less on nursing overnight, try adding other calming cues alongside feeding for 1–2 weeks, such as:
- white noise
- a consistent lullaby
- gentle rocking
- patting in the sleep space
Over time, these cues can help baby settle even if a night waking doesn’t always include a full feed.
7) Manage common sleep disruptors
- Teething: Gum pressure and drooling can disrupt sleep. Ask your clinician about appropriate comfort measures.
- Illness: Expect more waking. Focus on hydration and comfort; sleep often improves afterward.
- Congestion: A humidifier, saline drops, and upright cuddles can help some babies breathe easier (use medications only with clinician guidance).
Night Weaning: When It’s Possible, and When It’s Not the Right Fit
Night weaning means reducing or eliminating overnight feeds. It is not required for healthy sleep, and it isn’t appropriate for every baby at every age. Some breastfed babies naturally night wean; others don’t without a plan.
When night weaning may be considered
- Baby is older (often after 6 months, though some families wait longer)
- Baby is growing well and taking adequate daytime calories
- Night feeds seem more habitual/comfort-driven than hunger-driven
- Parents’ sleep deprivation is affecting health, safety, or mental well-being
Gentle night weaning approaches
- Shorten feeds gradually: reduce nursing time by a minute or two every few nights.
- Increase daytime feeds: offer more frequent nursing sessions earlier in the day.
- Change the order: feed, then use another soothing method to finish falling asleep.
- Partner support: if possible, a non-lactating caregiver can respond to some wakings so baby doesn’t automatically expect milk.
Important: If you night wean quickly, some parents notice breast discomfort or engorgement. Go slowly and monitor your comfort and supply.
Common Myths About Breastfed Baby Sleep
Myth: “Breastfed babies can’t sleep through the night.”
Many breastfed babies do sleep longer stretches, especially as they grow. Breastfeeding does not prevent healthy sleep; it may simply shape how and when babies wake in early months.
Myth: “If baby wakes, your milk isn’t filling enough.”
Night waking is rarely a sign of “bad” milk. Breast milk composition is well-suited to infant needs. Waking can be driven by development, comfort, or sleep cycles.
Myth: “Adding solids will fix sleep.”
Starting solids does not reliably lead to sleeping through the night. Some babies sleep a bit longer; many do not. Solids are primarily for exploration and gradual nutrition expansion in the early stages, not as a sleep tool.
A Practical, Parent-Friendly Plan (Start Here)
If you’re unsure what to do next, try this simple two-week plan. It respects breastfeeding, supports attachment, and often improves sleep without drastic changes.
Week 1: Set the foundation
- Get morning daylight exposure daily
- Keep nights dark and boring
- Use a consistent 10–20 minute bedtime routine
- Offer frequent daytime feeds (especially if baby is distractible)
- Choose one soothing cue to add every night (white noise or a lullaby)
Week 2: Nudge longer stretches gently
- Pause briefly when baby stirs to see if they resettle
- Try settling with your added cue before offering a feed for the first waking (if baby is calm and older than newborn stage)
- If you feed, keep it calm and return baby to sleep space promptly
- Adjust bedtime or naps by 15–30 minutes if overtiredness seems likely
If sleep worsens significantly, revert to what works and reassess. Many families benefit from individualized advice from a pediatric clinician, lactation consultant, or qualified infant sleep professional who supports breastfeeding.
The Bottom Line: When Do Breastfed Babies Sleep Through the Night?
Some breastfed babies start sleeping a 6–8 hour stretch by around 3–6 months, while others continue waking to feed well into the first year. Both patterns can be normal. The most helpful approach is to focus on safe sleep, strong daytime feeding, consistent routines, and gentle sleep-shaping strategies that support your baby’s development and your family’s well-being.
You’re not doing anything wrong if your breastfed baby still wakes. And you’re not asking too much if you need better rest. With a realistic plan and the right support, sleep usually improves—step by step.