What “Longer Stretches” Really Means
When parents ask, “When will my baby sleep longer at night?” they’re usually talking about a stretch that feels restorative—often 4–6 hours or more. In pediatric sleep research and clinical guidance, “sleeping through the night” can be defined more modestly, such as a baby sleeping a 6–8 hour stretch without signaling for help. That definition can surprise exhausted parents, but it reflects a key reality: infant sleep develops gradually, and wake-ups are normal for months.
It also helps to separate two concepts:
- Night sleep consolidation: longer continuous stretches at night.
- Night waking: babies may briefly wake between sleep cycles but not always cry or need feeding.
Many babies begin to connect sleep cycles more smoothly over time. Your goal isn’t perfection—it’s helping your baby get enough sleep safely while protecting your own well-being.
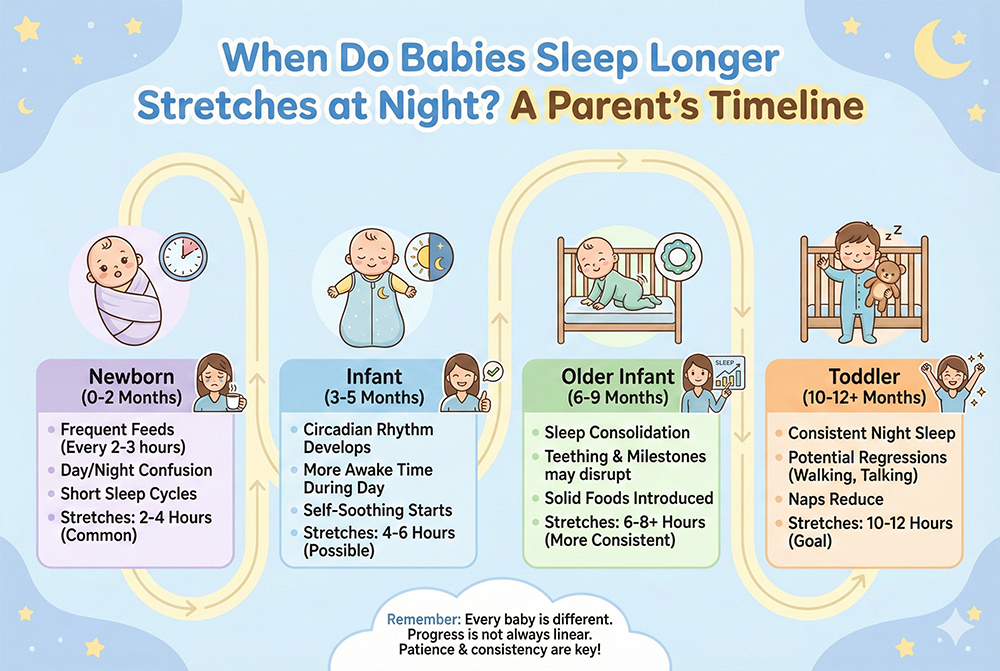
Typical Timeline: When Babies Start Sleeping Longer at Night
Every baby is different, but there are common developmental windows when longer stretches become more likely. Genetics, temperament, feeding method, medical factors, and sleep environment all influence the pace.
Newborns (0–8 weeks): 1–3 hour stretches are normal
Newborn sleep is driven mostly by the need to feed and by an immature circadian rhythm. Most newborns sleep in short bursts around the clock, often waking every 2–3 hours (sometimes more frequently). This is biologically normal and protective, especially for breastfeeding and weight gain.
What to expect:
- Sleep is highly variable and not “scheduled.”
- Day/night confusion is common.
- Cluster feeding in the evening can temporarily increase wakefulness.
2–3 months: Some longer stretches begin (3–5 hours)
Many babies start showing early circadian rhythm development around this time, with more sleep happening at night and slightly longer initial stretches. You may see a first “anchor” stretch after bedtime that is longer than the rest of the night.
What to expect:
- One longer stretch (often 3–5 hours) may appear.
- Bedtime may naturally shift earlier.
- Feedings are still common overnight and remain developmentally appropriate.
3–6 months: A common window for longer night sleep (5–8 hours)
This is the age range many parents notice real progress. For many infants, sleep cycles become more predictable and self-soothing skills begin to emerge (often supported by consistent routines). Some babies can sleep a 6–8 hour stretch, though many still need at least one night feed.
What to expect:
- Longer stretches become more common, especially if baby is growing well.
- One to two night feeds may still be normal.
- Sleep can temporarily worsen during growth spurts or developmental leaps.
6–9 months: Consolidation improves, but regressions are common
By this stage, many babies are capable of longer stretches, yet sleep may become disrupted due to increased mobility (rolling, crawling), separation anxiety, teething discomfort, illness, or changing nap needs. It’s common to see “two steps forward, one step back.”
9–12 months: Many can do 10–12 hours, but some still wake
Some babies sleep 10–12 hours at night with no feeds; others wake due to habit, temperament, hunger, or developmental changes. Both patterns can be normal if your baby is healthy and thriving.
Why Babies Wake Up at Night (Even When They’re “Old Enough”)
Night waking is not always a problem to fix—often it’s a normal part of infant physiology. Understanding the most common drivers can reduce stress and help you choose the right strategies.
1) Hunger and growth needs
Infants have small stomachs and high nutritional needs. Breastfed babies may wake more frequently than formula-fed babies, in part because breast milk is digested more quickly and feeding patterns vary. Frequent night feeds can also support milk supply.
2) Immature circadian rhythm
Melatonin production and mature day-night organization take time. Light exposure in the day and darkness at night gradually “set” the body clock.
3) Sleep cycle transitions
Babies have shorter sleep cycles than adults. Many wake briefly between cycles; if they rely on specific conditions (being rocked fully asleep, feeding to sleep, a pacifier that falls out), they may call for help to recreate them.
4) Developmental milestones and sleep regressions
Rolling, sitting, crawling, pulling to stand, and language bursts can temporarily disrupt sleep. So can separation anxiety, often peaking around 8–10 months.
5) Discomfort or illness
Reflux symptoms, eczema itch, congestion, ear infections, teething pain, or fever can all interrupt sleep. If sleep changes are sudden and severe, consider medical causes.
How Feeding Affects Longer Night Stretches
Parents often wonder if feeding method determines sleep. The relationship is nuanced: feeding affects waking patterns, but it doesn’t determine your baby’s ability to develop healthy sleep.
Breastfeeding and night sleep
Breastfed babies may feed more frequently overnight, especially in the early months. This can be normal and beneficial for growth and milk supply. Some breastfed babies still achieve long stretches by 3–6 months; others take longer.
Formula feeding and night sleep
Formula can sometimes support slightly longer stretches in some babies, but it’s not a guarantee. Babies may still wake out of habit, comfort needs, or developmental reasons.
Starting solids: does it help baby sleep longer?
Starting solids does not reliably make babies sleep through the night. Research and pediatric guidance generally suggest that solids are introduced around 6 months for developmental readiness and nutrition, not as a sleep strategy. Some families notice minor changes, but many do not.
What’s Normal vs. When to Check In With a Pediatrician
It’s reassuring to know that frequent night waking can be normal well beyond the newborn stage. Still, some patterns deserve a closer look.
Common “normal” patterns
- Waking every 2–4 hours in the first months.
- One to two night feeds at 4–8 months (sometimes more).
- Temporary sleep disruptions during milestones, travel, teething, or illness.
Consider checking in if you notice:
- Poor weight gain or fewer wet diapers than expected.
- Persistent snoring, gasping, or breathing pauses during sleep.
- Severe reflux symptoms (pain, arching, frequent vomiting, feeding refusal).
- Extreme irritability, inconsolable crying, or signs of significant pain.
- Sleep is suddenly much worse for more than 1–2 weeks without an obvious reason.
Safe Sleep Basics (Foundations Before Any Sleep Strategy)
Before focusing on longer stretches, ensure your baby’s sleep setup follows widely recommended safe sleep practices. This supports safer sleep and can also reduce unnecessary waking from discomfort.
- Back to sleep: Place baby on their back for every sleep.
- Firm, flat surface: Use a safety-approved crib, bassinet, or play yard with a firm mattress and fitted sheet.
- Keep the sleep space clear: No pillows, loose blankets, bumpers, or stuffed animals.
- Room-share, not bed-share when possible, especially in the first 6 months (often recommended up to 12 months).
- Avoid overheating: Dress baby appropriately; keep the room at a comfortable temperature.
If you use a swaddle, stop swaddling as soon as your baby shows signs of rolling.
Practical Tips to Help Babies Sleep Longer at Night
There’s no single trick that works for every baby, but the strategies below are evidence-informed and widely recommended in pediatric sleep guidance.
1) Support day-night rhythm
- Bright days: Get natural light exposure during morning and daytime hours.
- Dim evenings: Keep lights low and stimulation calm in the hour before bedtime.
- Night is boring: During nighttime feeds/diaper changes, use minimal light and minimal interaction.
2) Aim for age-appropriate wake windows (avoid overtiredness)
Overtired babies often wake more, not less. While exact wake windows vary, many babies sleep better when naps and bedtime align with their natural sleep pressure.
Signs your baby may be overtired: rubbing eyes, zoning out, fussiness, arching, “second wind” energy, short naps.
3) Create a simple, consistent bedtime routine
Routines cue the brain that sleep is coming. Keep it short and repeatable (15–30 minutes): bath (optional), pajamas, feeding, book/song, cuddle, into sleep space.
4) Feed well during the day
For many babies, getting adequate calories in daytime helps reduce night waking from hunger. If your baby is sleepy at feeds, ask your pediatrician or lactation consultant about techniques to keep feeds effective.
- Offer regular feeds during the day.
- Consider an earlier bedtime feed if evenings are hectic.
- Discuss “dream feeds” with your pediatrician if you’re considering them; they help some babies, not others.
5) Practice “drowsy but awake” when it works for your baby
Some babies do well being placed down sleepy but not fully asleep, which can build comfort with falling asleep in their sleep space. This is easier for many babies around 3–4 months and beyond, but it’s temperament-dependent. If it causes major distress, you can try a more gradual approach.
6) Give a brief pause before responding (when appropriate)
If your baby fusses lightly, pausing for 30–90 seconds can give them a chance to resettle. This is not about ignoring cries; it’s about noticing the difference between a full wake and a partial arousal. Always respond promptly if crying escalates or something seems wrong.
7) Optimize the sleep environment
- Dark room: Blackout curtains can help, especially in summer months.
- White noise: Can reduce wake-ups from household sounds; keep volume moderate and place the machine away from the crib.
- Comfortable temperature: Too hot or too cold can fragment sleep.
8) Consider how sleep associations affect wake-ups
If your baby always falls asleep while feeding, rocking, or with a pacifier, they may need help recreating that at each wake. You can keep these supports if they work for your family, or gradually shift them:
- Move feeding earlier in the routine so baby finishes feeding before being fully asleep.
- Try reducing rocking intensity over time (from rocking to still holding, then to crib soothing).
- If using a pacifier, consider offering it at bedtime but not repeatedly replacing it all night (depending on age and your comfort).
Night Weaning: When It Might Be Appropriate (and When It’s Not)
Night weaning means reducing or eliminating night feeds. It can support longer stretches for some babies, but it should match your baby’s growth, age, and medical context.
General considerations
- Many healthy babies still need night feeds in the first 6 months.
- Some babies can reduce night feeds earlier; others need them longer.
- Always consult your pediatrician if your baby was premature, has growth concerns, or has medical issues.
Gentle ways to reduce night feeds (if appropriate)
- Reduce duration/amount gradually: Shorten nursing time or reduce bottle volume over several nights.
- Increase daytime calories: Add an extra daytime feed if needed.
- Differentiate feeds from comfort: If baby wakes soon after a full feed, try soothing first, then feed if needed.
Common Sleep “Regressions” That Affect Longer Stretches
Sleep often changes in predictable windows. These are not permanent regressions, but periods of disruption.
Around 4 months
Sleep cycles mature and become more like adult patterns, which can lead to more frequent signaling between cycles. Consistent routines and gentle practice with independent settling (at your comfort level) often help.
Around 8–10 months
Separation anxiety and mobility can increase wake-ups. Extra reassurance at bedtime and consistent responses overnight can be helpful.
Toddlerhood (12+ months)
Teething, nap transitions, and boundary testing can impact sleep. At this age, clear routines and calm limits are often key.
A Realistic Night-Sleep Goal by Age
Instead of comparing your baby to others, consider a flexible target:
- 0–2 months: Any 2–3 hour stretch is normal; focus on safe sleep and recovery for parents.
- 2–3 months: A 3–5 hour first stretch may appear.
- 3–6 months: Many babies can achieve 5–8 hour stretches at times; some still wake more often.
- 6–12 months: Many can sleep 8–12 hours, though wake-ups can still occur.
If your baby is safe, growing well, and your family is coping, you are not “behind.”
Protecting Parental Sleep and Mental Health
Frequent night waking is one of the hardest parts of early parenting. Supporting your baby matters, but so does supporting you.
- Sleep shifts: If possible, trade a block of uninterrupted sleep with a partner or helper.
- Nap strategically: Even a short daytime nap can reduce burnout.
- Lower the bar: Simplify chores during tough weeks.
- Ask for help: If you feel persistently depressed, anxious, or hopeless, reach out to a healthcare provider. Postpartum mood and anxiety disorders are common and treatable.
Key Takeaways
Most babies start sleeping longer stretches at night between 3 and 6 months, but it’s normal for night waking to continue through the first year. Longer sleep depends on development, feeding needs, temperament, and consistent sleep cues. Focus on safe sleep, adequate daytime feeding, age-appropriate schedules, and gentle routines—and remember that progress is rarely linear.