Why Baby Poop Can Signal Dehydration
When you’re caring for a baby, diapers become a daily health report. While poop alone can’t diagnose dehydration, changes in stool alongside urine output, feeding, and behavior can offer important clues.
Dehydration happens when your baby loses more fluid than they take in. For infants, this can occur quickly—especially with vomiting, diarrhea, fever, hot weather, or feeding difficulties. Because babies have a higher body-water percentage and smaller fluid reserves than adults, even mild dehydration can become more serious in a short time.
Key takeaway: Baby poop changes can be a helpful early signal, but the most reliable diaper clue is often less urine. Look at the whole picture: poop, pee, feeding, energy level, and soft spot (fontanelle).
What Normal Baby Poop Looks Like (So You Can Spot Changes)
“Normal” varies by age and feeding method. Understanding typical patterns makes it easier to notice when something is off.
Breastfed baby poop
- Color: Mustard yellow, sometimes greenish
- Texture: Seedy, loose, or pasty
- Frequency: Often several times a day in early weeks; some older breastfed babies may go days between stools
Formula-fed baby poop
- Color: Tan, yellow-brown, or green
- Texture: Thicker, peanut-butter-like
- Frequency: Commonly 1–3 times per day, but can vary
Newborn transition stools
In the first days of life, poop changes from meconium (black, sticky) to greenish, then to yellow or brown as feeding establishes. This transition matters because persistent dark, sticky stools plus poor intake can sometimes signal feeding problems and risk for dehydration.
Starting solids
Once solids begin (often around 6 months), poop may become more formed, smell stronger, and change color based on foods eaten. This can be normal and not necessarily a sign of dehydration.
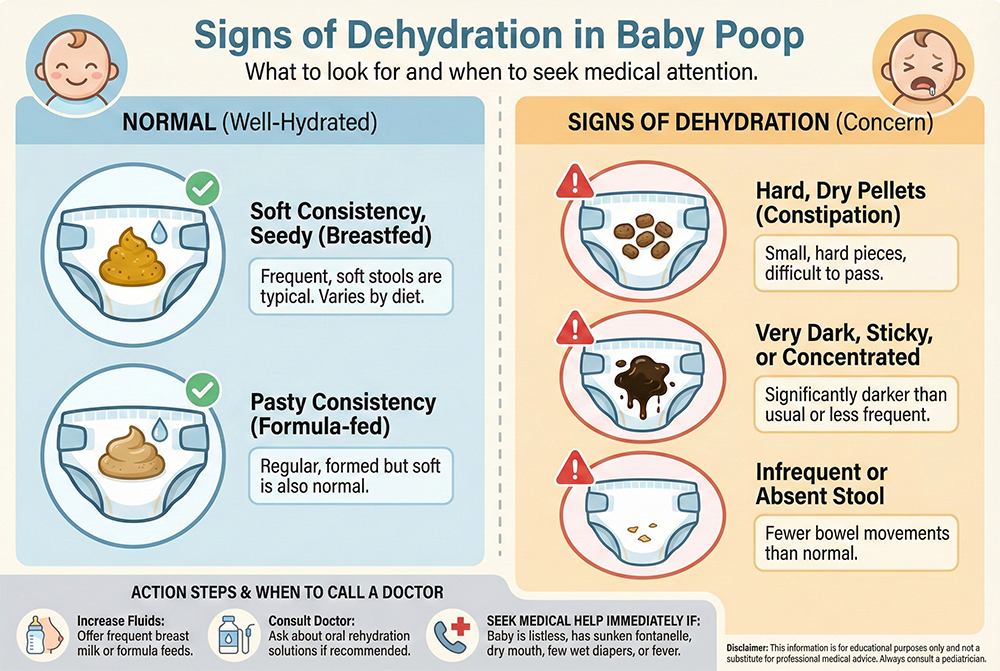
Signs of Dehydration in Baby Poop
Poop changes that may suggest dehydration usually relate to reduced water content in the stool or a digestive illness that’s causing fluid loss. Here’s what to watch for.
1) Hard, dry, pellet-like stools
One of the most common poop-related clues is constipation-style stool: small, hard pellets or a firm log that’s difficult to pass. Dehydration can contribute because the colon absorbs more water from stool when the body is trying to conserve fluids.
What you might notice: straining, discomfort, fussiness during bowel movements, or a small amount of blood on the stool from a tiny anal fissure (a small tear), which can happen with hard stools.
Important: Straining alone does not always mean constipation in young infants—many babies grunt and strain even with soft stools. The texture matters most.
2) Less frequent stooling with harder texture (especially after illness)
If your baby recently had fever, vomiting, or diarrhea and now has fewer bowel movements with thicker, drier stools, that combination can reflect overall reduced fluid intake or ongoing mild dehydration.
3) Diarrhea (watery stools) that increases dehydration risk
Watery stools don’t “look dehydrated,” but they can cause dehydration quickly because they represent fluid loss. Diarrhea is typically defined by a sudden increase in stool looseness and/or frequency compared to your baby’s usual pattern.
Red flag pattern: multiple watery stools in a day, especially if paired with vomiting, fever, poor intake, or fewer wet diapers.
4) Very dark stool with other dehydration symptoms
Stool color can vary widely and isn’t a perfect hydration marker. However, if stool looks unusually dark and your baby is feeding poorly with reduced urine output, it’s worth paying closer attention. Dark stool can have many causes, including iron supplementation or formula, certain foods (in older babies), or gastrointestinal bleeding. If stool is black and tarry (after the newborn meconium period), seek medical guidance promptly.
5) Mucus or blood with diarrhea
Mucus strands or blood in the stool can occur with infections, milk protein intolerance, or irritation. If diarrhea is present, fluid losses can be significant. Blood or mucus doesn’t equal dehydration on its own, but it raises concern for an underlying cause that may increase dehydration risk.
Other (More Reliable) Dehydration Signs to Check Alongside Poop
If you suspect dehydration based on stool changes, confirm by checking these more dependable signs. Parents often find it helpful to do a quick “diaper and behavior” checklist.
Wet diaper changes
- Fewer wet diapers: A major warning sign. Many babies should have regular wet diapers across the day; fewer than usual is concerning.
- Darker, strong-smelling urine: Can indicate more concentrated urine.
Mouth, tears, and skin
- Dry mouth or lips
- Fewer tears when crying (in babies who typically produce tears)
- Cool, mottled extremities or less elastic skin (in more significant dehydration)
Fontanelle (soft spot) and eyes
- Sunken soft spot (fontanelle)
- Sunken eyes
Behavior and feeding
- Sleepier than usual, hard to wake, or unusually irritable
- Feeding less or refusing breast/bottle
- Rapid breathing or rapid heartbeat (more urgent sign)
What Causes Dehydration in Babies?
Knowing the common triggers helps you act quickly and prevent dehydration from worsening.
Illness-related fluid loss
- Stomach bugs: vomiting and diarrhea can drain fluids quickly
- Fever: increases insensible water loss
- Respiratory illness: faster breathing and poor feeding can reduce intake
Feeding challenges
- Breastfeeding difficulties: shallow latch, low milk transfer, or delayed milk supply
- Not taking enough formula: illness, bottle refusal, incorrect mixing, or infrequent feeds
Heat exposure
Hot environments can increase fluid needs. Babies can’t regulate temperature as efficiently as adults, and overheating can contribute to dehydration risk.
Age-by-Age Considerations: Newborns vs. Older Babies
Newborns (0–8 weeks)
Newborns are especially vulnerable. In the early days, diaper counts help track adequate intake. If stools are not transitioning from meconium, or if wet diapers are fewer than expected, contact your pediatrician or lactation consultant promptly. Newborn dehydration can become serious quickly.
Infants (2–6 months)
At this stage, babies often have a more predictable feeding rhythm. Watch for a noticeable change: fewer wet diapers, decreased feeding time/volume, or lethargy—especially during illness.
Older babies (6–12 months)
With solids, poop naturally becomes more formed. Constipation can happen even with normal hydration, but hard, dry stools plus decreased urine or poor intake is more concerning. At this age, your baby may sip small amounts of water with meals if advised by your pediatrician, but breast milk/formula remains the primary fluid source.
What to Do If You Think Your Baby Is Dehydrated
If stool changes make you suspect dehydration, focus on restoring fluids safely and watching for red flags.
Offer frequent feeds
- Breastfed: Nurse more often. Even short, frequent feeds can help.
- Formula-fed: Offer smaller, more frequent bottles if your baby is refusing full feeds.
Consider oral rehydration solution (ORS) during vomiting/diarrhea
For babies with significant vomiting or diarrhea, pediatricians often recommend an oral rehydration solution (ORS) rather than plain water. ORS contains the right balance of glucose and electrolytes to improve absorption.
How to give it: Small amounts frequently (for example, a teaspoon or small sips every few minutes) can be easier to keep down than larger volumes.
Always follow your pediatrician’s guidance on whether ORS is appropriate for your baby’s age and situation.
Avoid common pitfalls
- Avoid giving plain water to young infants unless your clinician advises it. Too much water can disrupt electrolyte balance.
- Do not dilute formula to “add fluids.” Dilution can be unsafe and reduce calorie intake.
- Avoid sugary drinks (juice, soda) for rehydration—these can worsen diarrhea.
Track diapers and symptoms
Write down:
- Number of wet diapers
- Number and type of stools (watery vs. formed)
- Vomiting episodes
- Fever readings
- Approximate feeds taken
This information helps your pediatrician assess severity and next steps.
When to Call the Pediatrician (and When to Seek Urgent Care)
Trust your instincts—if your baby seems “not right,” it’s always reasonable to call for advice.
Call your pediatrician promptly if you notice:
- Diarrhea lasting more than a day (or sooner in young infants)
- Repeated vomiting
- Fever (especially in babies under 3 months)
- Hard stools with significant discomfort or blood
- Fewer wet diapers than usual
- Refusing feeds or taking much less than normal
Seek urgent care/emergency evaluation if your baby has:
- Very sleepy, difficult to wake, or unusually limp
- Signs of moderate to severe dehydration: very dry mouth, no tears, sunken eyes, sunken fontanelle, markedly reduced urine
- Persistent vomiting and can’t keep fluids down
- Blood in stool with illness symptoms or black/tarry stool (after the newborn period)
- Breathing difficulty, bluish lips, or severe weakness
Preventing Dehydration: Practical, Parent-Friendly Tips
Many dehydration episodes are linked to illness, but there are simple ways to reduce risk and catch problems early.
Keep feeding consistent
- Offer feeds more often during growth spurts, hot weather, and mild illness.
- If breastfeeding is painful or baby seems frustrated at the breast, seek lactation support early.
Use diaper patterns as your daily dashboard
Get familiar with your baby’s “normal.” A sudden change—especially fewer wet diapers—deserves attention even if poop changes are subtle.
Support healthy poop with appropriate nutrition
- For babies on solids: offer fiber-rich options (pureed prunes, pears, peaches, peas) if constipation is an issue.
- Balance binding foods (banana, rice cereal) with fruits/vegetables if stools become hard.
- Continue breast milk or formula as the main fluid source through the first year, unless advised otherwise.
Manage illness proactively
- Dress baby in breathable layers and keep room temperature comfortable during fever.
- Offer smaller, more frequent feeds when appetite is low.
- Ask your pediatrician about ORS early if vomiting/diarrhea begins.
Common “Poop Confusers” That Aren’t Always Dehydration
Some stool changes look alarming but may be unrelated to hydration.
Green poop
Green stools can be normal in formula-fed babies, during mild illness, or after certain foods (older babies). Hydration status depends more on wet diapers and overall behavior.
Thicker poop after starting solids
More formed stools can be normal with solids. Focus on whether stool is hard and difficult to pass versus simply more “adult-like.”
Iron-related dark stools
Iron-fortified formula or supplements can darken stools. If your baby otherwise seems well and diaper output is normal, this is often expected. If stool is black and tarry or your baby seems unwell, contact your clinician.
A Calm, Simple Checklist for Parents
If you’re scanning diapers and wondering about dehydration, use this quick summary:
- Poop clues: hard, dry pellets; constipation after illness; watery diarrhea that’s frequent
- Pee clues: fewer wet diapers; darker urine
- Body clues: dry mouth, fewer tears, sunken soft spot
- Behavior clues: poor feeding, unusual sleepiness, extreme fussiness
If multiple categories are affected, it’s time to call your pediatrician for guidance.
Final Thoughts
Baby poop can provide helpful hints about hydration—especially when stools become unusually hard and dry or when diarrhea increases fluid loss. Still, the most important signs of dehydration are often reduced urine output, poor feeding, and changes in alertness. When in doubt, reach out to your child’s healthcare provider. You’re not overreacting—early action is one of the best protections for your baby’s health.